What is Bone Age?
Bone age is a measure of the degree of skeletal maturity of a child, i.e. how far the child has advanced in its development of the skeleton. Conventionally this is determined from an X-ray image of the hand.
----- Analyse your own bone age image using this Online tool -----
Hormones control skeletal maturation, and the same hormones also govern the timing of puberty. So a child with delayed skeletal maturity is also likely to have puberty late, e.g. late menarche.
Bone age is measured in years, most often using the Greulich-Pyle scale. If a child has bone age 10 years, it means that the child maturation is as advanced as the average of the 10-year old children from Ohio in 1930-1940 that Greulich and Pyle studied.
Different population groups mature at different speeds. For instance, healthy children mature faster than children living under poor conditions. Present-day Western-European children mature approx. 2-4 months later than the very healthy children studied by Greulich and Pyle. Therefore, the average bone age of 10-year-old children is approx. 9.7 years.
The standard deviation of bone age at a given age is approx. 1 year. This implies that in a random group of 7 boys of the same age, there is on average 3 years difference between the most and the least mature boy. I.e. the most advanced boy hits puberty 3 years before the least advanced.
The growth spurt of boys occurs on average at 14.2 years of bone age. Girls on the other hand have menarche at bone age 13.2 years, on average.
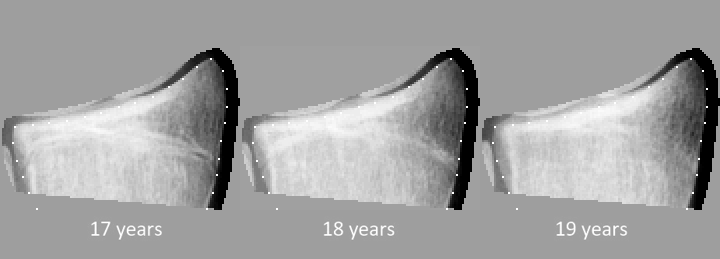
The following illustrations show a series of images from the first Zurich Longitudinal Study (courtesy of Zurich Univ) show annual X-rays of the same bone.
Maturation of the third metacarpal
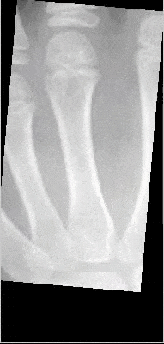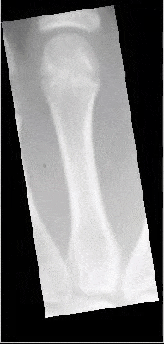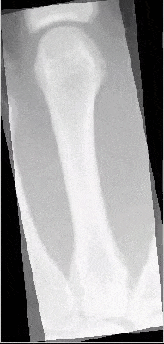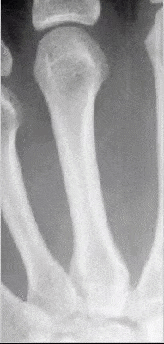
Maturation of the third proximal phalanx
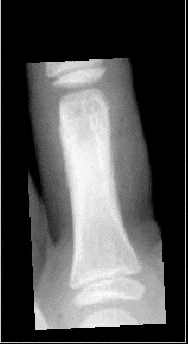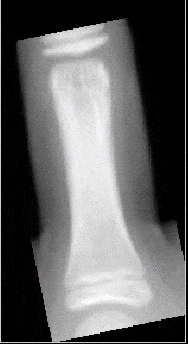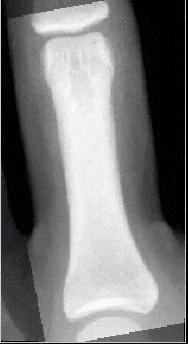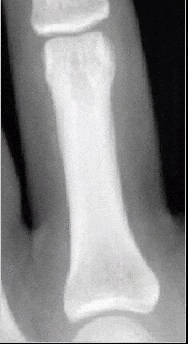
The BoneXpert Technology
BoneXpert analyses the image completely automatically, independently of the rotation of the hand. Both left and right hands are accepted.
BoneXpert analyses the following 21 bones: Radius, ulna, metacarpals, and phalanges. These are used for the overall bone age formed as a simple average over these 21 bones.
In addition, the seven carpals are considered, and a carpal bone age is computed for the group of all visible carpals. Thus the carpal bone age is not "mixed into" the overall bone age. Carpal bone age is usually not determined for boys with bone age above 12 y and for girls with bone age above 10 y, because the carpals develop very little above these bone ages.
The image analysis of the 21 bones is divided into three layers (this figure is from the first BoneXpert publication from 2009 - at that time only 13 bones were analysed, but the architecture is the same today)
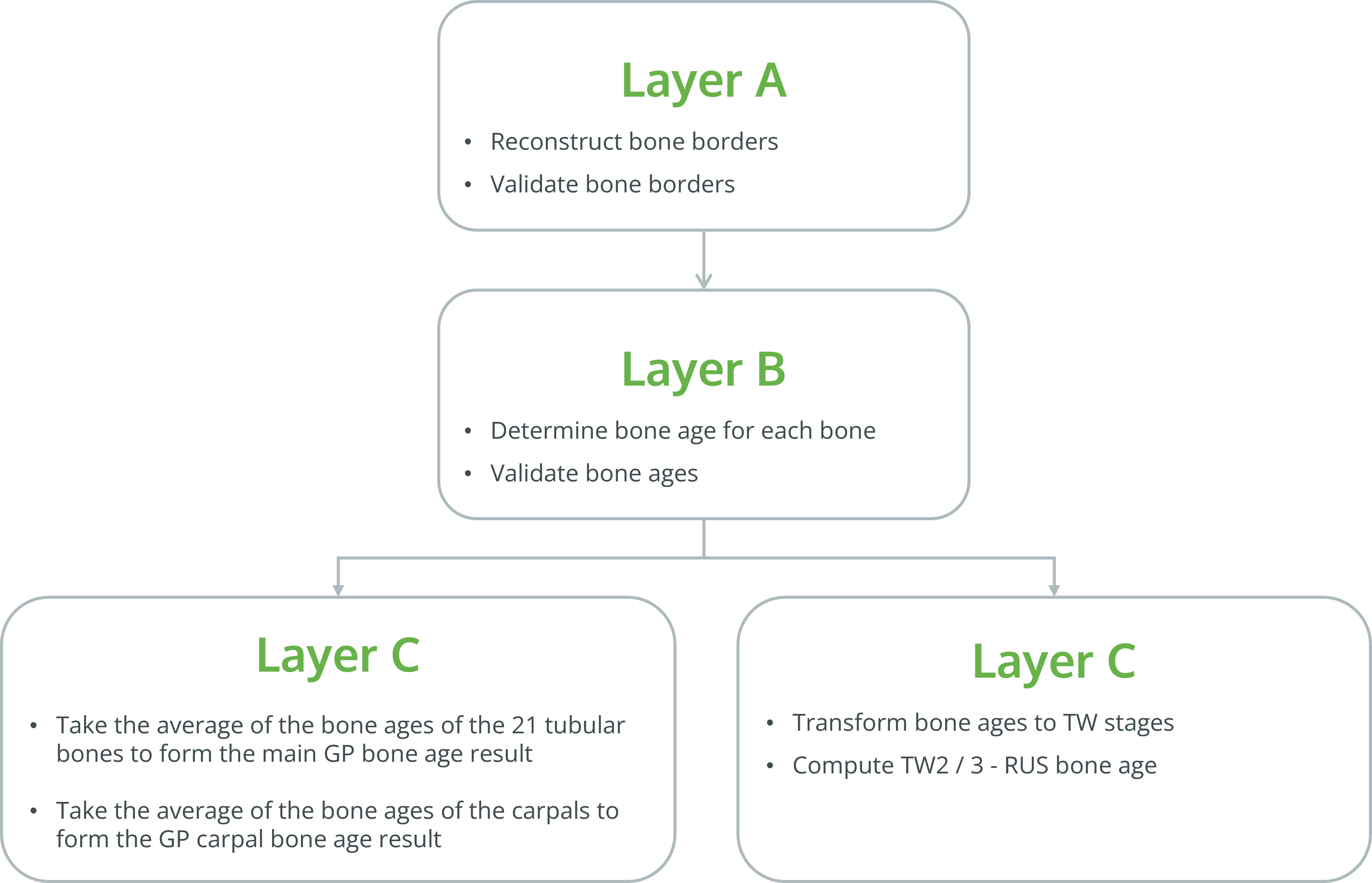
In Layer A, the borders of the bones are found using a sophisticated algorithm developed by machine learning. It is a combination of supervised and unsupervised machine learning, which has learned to locate landmarks on the bones and learned the allowed shape of each bone. This allows level A to locate each bone and reject it, if it is not in accordance with the model. A recent overview of methods of this kind can be found here. Although BoneXpert is a prominent example of artificial intelligence (AI), it differs in two ways from many recent AI methods: (1) It does not learn continuously when it runs in "production" in a hospital. (2) The image analysis is performed inside the hospital, rather than in the cloud, so the images never leave the hospital.
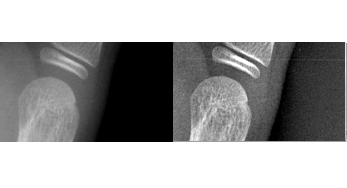
BoneXpert’s shape model for the third proximal phalanx of 13-17 year old boys

BoneXpert’s shape model for the third proximal phalanx of 7-13 year old boys

Adult Height Predictor
 The BoneXpert adult height prediction (AHP) method is a modernisation of the classical Bayley-Pinneau method from 1952.
The BoneXpert adult height prediction (AHP) method is a modernisation of the classical Bayley-Pinneau method from 1952.
Like the Bayley-Pinneau method, it is intended for normal, non-pathological untreated children
From gender, age, height and bone age, it predicts the adult height. Optionally, one can enter parental height, which improves the accuracy.
The uncertainties of the predictions of adult height are given as a standard deviation (±SD), i.e. the true values will be within the indicated range with 68% probability.
The predictor is intended to be used with Greulich-Pyle (GP) bone age determined by BoneXpert; however, it can also be used with manual GP bone age, but the uncertainties of the predictions are then considerably larger than indicated, due to the rater variability.
The tool implements the most accurate statistical model, but is not in itself a diagnostic tool, and it should not be used without consulting a pediatric endocrinologist or another medical expert.
Four different adult height predictions
The tool provides four different predictions, which all depend on the assumed population height.
The most accurate prediction is highlighted in green and it is the one which is shown on the growth chart.
- AHP(x-ray) based on age, bone age and height
- AHP (parental) based solely on the parents’ heights.
- AHP(x+p) based on age, bone age, height and parental height
- AHP(x+m) only for females - based on age, bone age, height and height at menarche
A large discrepancy between AHP(x-ray) and AHP(parental) indicates that the child grows differently from what is expected from its parental heritage, i.e. it could be a sign of disorder.
The Age of Peak Height Velocity (APHV) and the growth path
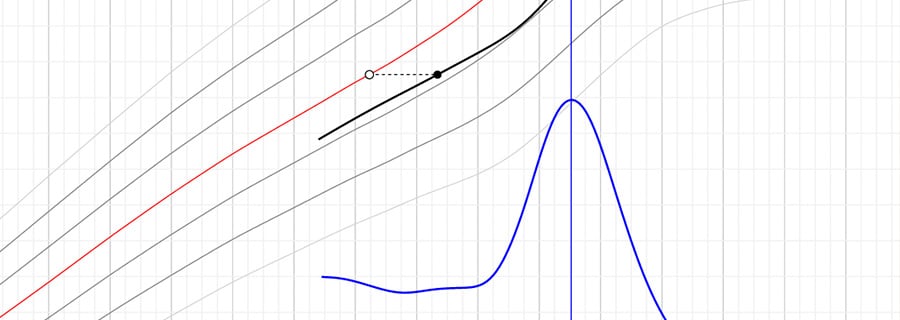
For Caucasian children, the tool also predicts the APHV, and based on that it draws the most likely growth path from the current height to the predicted adult height in a growth chart.
The population groups
The AHP depends on the ethnicity, and within each ethnicity it depends on the assumed population height. One can choose among several population groups.
An important feature of the tool is that it computes Standard Deviation Scores (SDS) of bone age and Bone Health Index (BHI). The choice of population affects these SDS values.
Examples:
BA SDS = -1.0 means that the child's bone age is one SD below the mean for children of the same age
BHI SDS = -2.0 means that the child's BHI is two SDs below the mean for children of the same bone age
Bone Health Index
BoneXpert measures the amount of cortical bone in the metacarpals by the Bone Health Index (BHI). BHI is part of the CE-marked medical device, i.e. it is cleared for routing clinical use in Europe.
BHI is based on measurements of cortical thickness, T, in the three middle metacarpals. This is one of the oldest methods to assess bone mass, and it was popular in the 1960’s where T was measured directly on the X-ray films, typically in the middle of the second metacarpal. BoneXpert performs 100 independent measurements of T in three regions of interest (indicated to the right), thereby obtaining a much better precision than the old manual method.
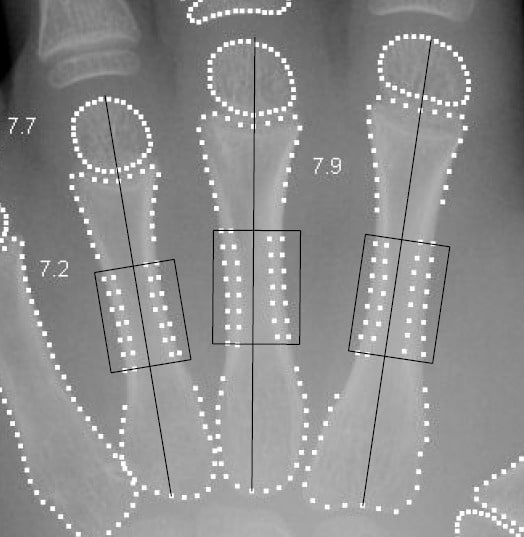
Several measures for bone health have been used in the past. Some have used T directly, and others have preferred the metacarpal index 2T/W, where W is the bone width. Finally Exton-Smith used T/L, where L is the bone length.
BoneXpert’s BHI does something in between, using BHI approximately proportional to T / (LW)0.33. As explained at great length here, this BHI formula was designed to provide the optimal compensation for the highly variable size and proportion of children.
The exact definition is BHI = π T (1 − T/W) / (LW)0.33
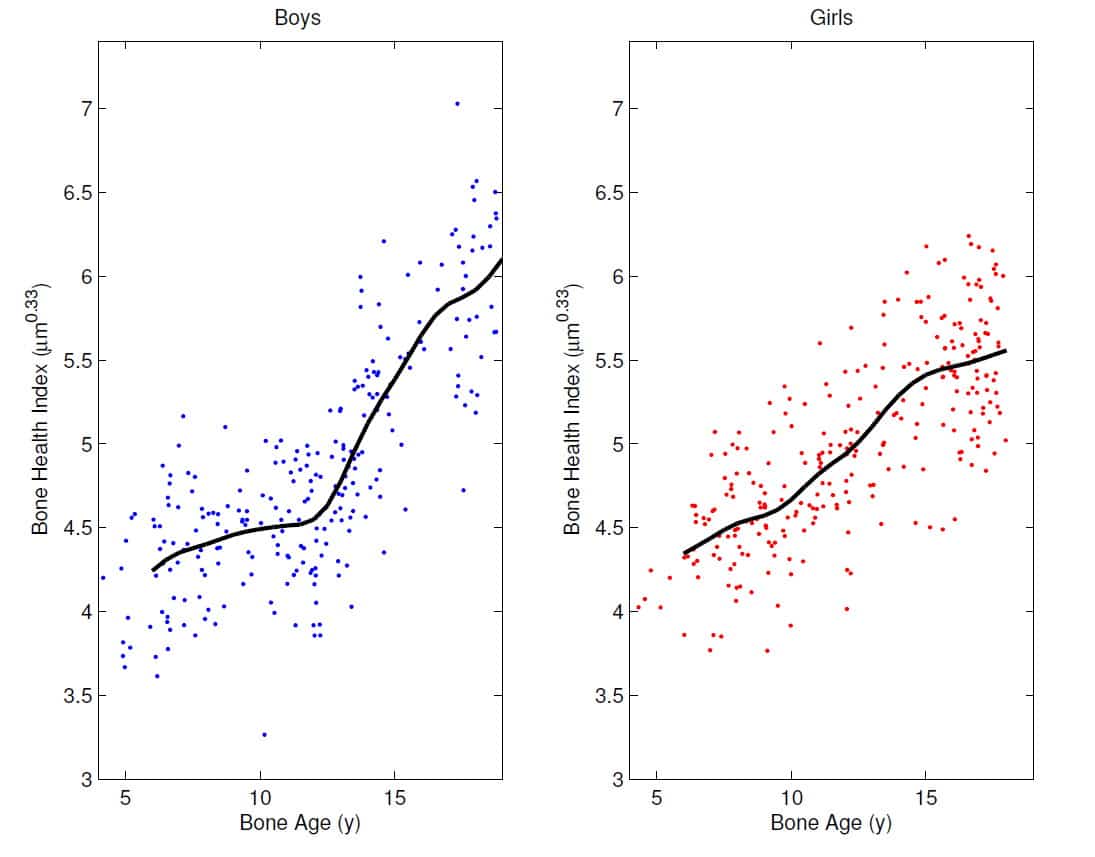
The figure above shows the BHI reference curve, i.e. the average BHI versus bone age, constructed from healthy Dutch children studied in 1997. BoneXpert computes BHI standard deviation scores (SDS) accordingly. Notice the rapid increase of BHI at puberty, illustrating the importance of assessing BHI as a function of bone age rather than age.
As a result of the large number of measurements underlying BHI, its precision (coefficient of variation, or CV) is 1.4% at age 10. This error is due mainly to variations in the way the hand is placed on the imaging detector. Since the standard deviation of BHI at fixed bone age is 7.5%, this CV corresponds to a precision of BHI of 0.19 SDs, or 0.19 units of BHI-SDS.
In growth hormone deficient children it was found that BHI-SDS increases on average 0.74 in the first year of treatment, which means that this change can be readily measured in the individual child (see DD Martin, C Heckmann, MB Ranke, G Binder, HH Thodberg, Differentiation of GH effects on metacarpal bone in children with GHD, ICCBH5, Cambridge, UK. June 23-26, 2009 Bone, Volume 45, Page S60)
BoneXpert automatically rejects the BHI determination if the bones are reconstructed inconsistently, or if the image quality is insufficient, e.g. due to blur of lack of contrast.